If you’re struggling with Achilles tendon pain, you’ve probably encountered conflicting advice that leaves you more confused than when you started. Unfortunately, several persistent myths about Achilles tendinopathy continue to mislead patients and even some healthcare providers, often making recovery longer and more difficult than necessary.
This comprehensive guide examines five of the most dangerous misconceptions about Achilles tendon treatment, explains why they’re harmful, and reveals what current research actually tells us about effective recovery strategies.
Myth #1: Complete Rest Is the Best Medicine for Achilles Pain

The Dangerous Belief
Many people believe that completely avoiding all activity and “resting” an injured Achilles tendon will allow it to heal naturally. This seems logical – if movement hurts, stopping movement should help, right?
Why This Approach Backfires
While this myth originated from reasonable medical principles used for acute injuries, complete rest actually weakens tendons over time. Research has consistently shown that tendons need mechanical loading to maintain their strength and structure.
When you completely rest an Achilles tendon:
- Collagen production decreases significantly
- The tendon loses its ability to handle normal daily stresses
- Muscle strength in the calf complex deteriorates
- Return to activity becomes even more challenging
The Evidence-Based Alternative: Modern tendinopathy research supports a “load management” approach. This means finding the sweet spot where you’re doing enough activity to stimulate healing without overwhelming the tendon’s current capacity.
Myth #2: Achilles “Tendinitis” Is an Inflammatory Condition
The Persistent Misconception
For decades, Achilles tendon problems were labeled “tendinitis,” leading to treatments focused on reducing inflammation through ice, anti-inflammatory medications, and cortisone injections.
What Research Actually Reveals
Groundbreaking studies by Khan, Cook, and other tendon researchers in the 2000s fundamentally changed our understanding. Chronic Achilles tendinopathy is primarily a degenerative condition, not an inflammatory one.
The key findings:
- Chronic overuse tendon injuries show an absence of active inflammation
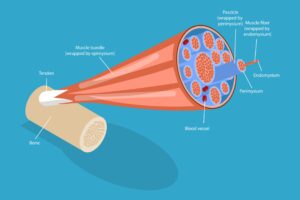
- Instead, tendons develop microtears and disorganized collagen
- Pain doesn’t correlate directly with inflammation or visible damage
- Anti-inflammatory treatments often fail to address the root problem
Why the terminology matters: This is why experts now prefer “tendinopathy” over “tendinitis” – it more accurately reflects the degenerative nature of the condition.
Myth #3: Cortisone Injections Provide a Quick Fix
The Tempting “Solution”
Corticosteroid injections often provide rapid pain relief, leading many to believe they’ve found a cure for their Achilles problems. The immediate improvement can be dramatic, making this treatment seem like a miracle solution.
The Hidden Long-Term Consequences
While cortisone shots may provide excellent short-term pain relief, research shows they often worsen outcomes in the long run. Here’s why:
- Steroids have a catabolic effect on tendon cells, actually inhibiting collagen repair
- Long-term follow-up studies show patients fare worse months later compared to conservative treatments
- There’s an increased risk of Achilles tendon rupture following steroid injections
- The pain relief can mask ongoing tendon weakness, leading to overuse
Current Expert Consensus: Most sports medicine professionals now reserve steroid injections for Achilles problems only in rare cases, if at all, emphasizing rehabilitation exercise as the primary treatment.
Myth #4: The Alfredson Eccentric Protocol Works for All Achilles Problems

The Oversimplified Approach
The landmark 1998 study by Håkan Alfredson showing remarkable success with eccentric heel-drop exercises was revolutionary. However, this led to the belief that the same protocol should be applied to all Achilles tendon problems.
Why Location Matters Critically
Later research revealed a crucial distinction that many practitioners initially missed:
Mid-portion Achilles tendinopathy (pain in the middle of the tendon) responds well to traditional eccentric heel drops with excellent outcomes.
Insertional Achilles tendinopathy (pain where the tendon attaches to the heel bone) can actually be worsened by heel drops below step level. A 2008 study by Jonsson et al. found:
- 67% success rate when avoiding dorsiflexion beyond neutral
- Only 28% success rate with traditional heel drops into full stretch
The reason: Dropping the heel below the step compresses the tendon against the heel bone, which is problematic when the insertion point is already irritated.
Myth #5: All Pain Means You’re Causing Damage

The Fear-Based Approach
Many people with Achilles problems become afraid of any discomfort, interpreting pain as a sign that they’re making the injury worse. This leads to excessive avoidance of activity and over-reliance on supports.
Understanding Productive vs. Destructive Pain
Modern pain science shows that not all pain equals damage, especially in chronic tendinopathy. The key is learning to distinguish between different types of pain:
Acceptable pain during rehab:
- Mild to moderate discomfort during exercise
- Soreness that returns to baseline within 24 hours
- No significant increase in morning stiffness the next day
Warning signs to respect:
- Sharp, severe pain during activity
- Pain that significantly worsens after exercise
- Persistent increased pain lasting more than 24 hours
The 24-hour rule: If an activity causes tolerable pain that settles back to baseline within 24 hours, that activity is generally considered safe and beneficial for tendon adaptation.
The Truth About Orthotics and Heel Lifts
The Overreliance Problem
While research shows that heel lifts and orthotics can reduce Achilles tendon loading, some people interpret this as a standalone solution. The misconception is that simply reducing load will cure the problem.
Why Support Alone Isn’t Enough
Temporary offloading has its place, but orthotics alone are not very effective for treating Achilles tendinopathy. Here’s why:
- Supports don’t address the underlying tendon pathology
- Constant external support can lead to detraining of the calf muscles
- The tendon still needs progressive loading to remodel and strengthen
- Over-reliance can shift stress to other areas, potentially causing new problems
The balanced approach: Use supportive devices as temporary aids to manage pain and allow activity, but combine them with active rehabilitation exercises.
What Actually Works: Evidence-Based Achilles Tendon Recovery
Current best practices for Achilles tendinopathy represent a more balanced, evidence-based approach:
Load Management (Not Complete Rest)
Find the “loading sweet spot” where you’re doing enough activity to stimulate healing without overwhelming the tendon’s current capacity.
Progressive Strengthening
Focus on tendon conditioning through gradually increasing loads, whether through eccentric, concentric, or isometric exercises – the progressive loading is more important than the specific type of contraction.
Location-Specific Treatment
Customize your approach based on whether you have mid-portion or insertional Achilles tendinopathy, as they require different exercise modifications.
Pain Monitoring (Not Fear)
Use pain as a guide to modify activities, but don’t let fear of discomfort prevent appropriate loading of the tendon.
Holistic Approach
Address contributing factors like calf weakness, biomechanical issues, and training errors alongside direct tendon treatment.
Key Takeaways for Your Achilles Recovery

The journey from myth to evidence-based treatment represents a significant evolution in our understanding of Achilles tendinopathy. The most important lessons are:
- Avoid black-and-white rules – Recovery is nuanced and individual
- Focus on progressive loading – Your tendon needs appropriate challenge to adapt
- Understand your specific condition – Mid-portion and insertional problems require different approaches
- Be patient with the process – Tendon healing takes time, but proper treatment works
- Seek qualified guidance – Work with healthcare providers who understand current tendinopathy research
By understanding these myths and embracing evidence-based treatment, you can avoid the frustrating cycles of failed treatments and move toward genuine recovery. Remember, the goal isn’t just to eliminate pain – it’s to build a tendon that can handle the demands of your active life.