When research findings are misinterpreted, patients suffer. Much like the infamous “knees over toes” myth that misled athletes for decades, Achilles tendinopathy treatment has been plagued by similar misconceptions. These misinterpretations have led many down ineffective treatment paths, prolonging recovery and sometimes worsening outcomes. This comprehensive guide examines how research on Achilles tendon pain has been misunderstood and what current evidence actually tells us about effective treatment approaches.
| Contents | Jump to Section |
| The “Just Rest It” Fallacy | Read More |
| The “Tendinitis” Mislabeling | Read More |
| Corticosteroid Injection Risks | Read More |
| Eccentric Exercise Misapplication | Read More |
| Pain Avoidance Misconception | Read More |
| Overreliance on Passive Treatments | Read More |
| Evidence-Based Approaches | Read More |
| Conclusion | Read More |
The “Just Rest It” Fallacy: Why Complete Rest Hinders Recovery
For decades, the standard advice for Achilles tendon pain was simple: rest until it feels better. This approach seemed logical – if loading causes pain, then removing all load should allow healing. Unfortunately, this oversimplification has led countless patients down a path of prolonged recovery and recurring symptoms.
Origin of the Myth
The “just rest it” approach originated from early rehabilitation protocols that treated Achilles pain as an acute inflammatory condition. Medical textbooks from the 1970s and 1980s commonly recommended immobilization and complete rest for tendon injuries. This advice was based on limited understanding of tendon biology and healing processes, along with short-term studies showing initial pain relief with rest.
Why Complete Rest Is Problematic
Modern research has revealed that tendons require mechanical stimulation to maintain their structure and function. When a tendon is completely unloaded for extended periods, several negative adaptations occur:
Tendon Deconditioning
- Collagen synthesis decreases
- Tendon stiffness reduces
- Load tolerance diminishes
- “Stress-shielding” weakens structure
Muscle Adaptations
- Calf muscle atrophy
- Neuromuscular inhibition
- Reduced force production
- Altered movement patterns
Research by Magnusson and Kjaer demonstrated that complete tendon unloading leads to decreased collagen synthesis and reduced tendon cross-sectional area – essentially making the tendon weaker. This explains why many patients who followed strict rest protocols often experienced temporary relief, only to have symptoms return (often worse) upon resuming activity.
“Recent evidence suggests that complete rest can actually hinder recovery. Tendons need appropriate mechanical loading to stimulate repair and remodeling processes.”
— British Journal of Sports Medicine, 2018
The Modern Approach: Load Management
Current best practice has shifted from complete rest to strategic load management. This involves:
- Temporarily reducing activities that provoke significant pain
- Maintaining some level of tendon loading within pain tolerance
- Gradually increasing load as symptoms improve
- Implementing progressive strengthening exercises
- Monitoring response to load (pain patterns, morning stiffness)
This approach recognizes that tendons need mechanical stimulation to adapt and strengthen. The key is finding the “sweet spot” of loading – enough to stimulate repair without overloading and causing further irritation.
The “Tendinitis” Mislabeling: Inflammation vs. Degeneration
Perhaps the most fundamental misunderstanding in Achilles tendon pathology has been the nature of the condition itself. For years, painful Achilles tendons were diagnosed as “tendinitis” – implying that inflammation was the primary problem. This mischaracterization led to treatment approaches that often missed the mark.
Origin of the Inflammation Model
The term “Achilles tendinitis” became standard medical terminology based on early observations of some inflammatory cells in acute tendon injuries. Medical education reinforced this model, teaching that tendon pain was primarily an inflammatory condition requiring anti-inflammatory treatments. This led to widespread use of ice, NSAIDs (like ibuprofen), and even cortisone injections as first-line treatments.
The Degenerative Reality
Groundbreaking research in the late 1990s and early 2000s by Khan, Cook, and others revealed a surprising truth: chronic Achilles tendinopathy shows little to no active inflammation. Instead, biopsies of painful tendons revealed:
- Disorganized collagen fiber structure
- Increased ground substance (proteoglycans)
- Abnormal cell populations and activity
- Increased tendon thickness
- Neurovascular ingrowth (new blood vessels and nerves)
These findings represented a failed healing response and tissue degeneration rather than classic inflammation. This discovery prompted a terminology shift from “tendinitis” to “tendinopathy” – acknowledging that the “-itis” suffix (meaning inflammation) was inaccurate for most chronic cases.
Terminology Matters
The shift from “tendinitis” to “tendinopathy” isn’t just semantic – it reflects a fundamental change in how we understand and treat the condition. Tendinopathy acknowledges that the primary issue is degenerative changes in tendon structure rather than simple inflammation.
Implications for Treatment
Understanding that Achilles tendinopathy is primarily degenerative rather than inflammatory has profound treatment implications:
| Old Approach (Inflammation Model) | Current Approach (Degeneration Model) |
| Focus on reducing inflammation | Focus on stimulating tissue repair and adaptation |
| Emphasis on rest and anti-inflammatories | Emphasis on appropriate loading and exercise |
| Short-term symptom relief prioritized | Long-term tendon capacity building prioritized |
| Pain viewed as direct indicator of damage | Pain recognized as complex and not always proportional to tissue state |
This paradigm shift explains why anti-inflammatory approaches often provided only temporary relief without addressing the underlying problem. Modern treatment now focuses on stimulating tendon adaptation through appropriate loading rather than simply calming inflammation.
Corticosteroid Injection Risks: Short-Term Relief, Long-Term Consequences
Corticosteroid (cortisone) injections have been widely used for Achilles tendon pain, often promoted as a quick solution. While these injections can indeed provide rapid pain relief, research has revealed concerning long-term consequences that patients should understand.
The Allure of Quick Relief
Steroid injections gained popularity because they often provide dramatic short-term pain reduction. Early case reports and clinical experience showed that patients frequently experienced significant relief within days of injection. This immediate benefit made steroid shots an attractive option for both patients seeking fast results and clinicians looking to provide rapid symptom management.
The Research Reality
Longer-term studies have revealed a troubling pattern. A systematic review published in The Lancet found that while corticosteroid injections often provided superior pain relief in the first 4-8 weeks compared to other treatments, outcomes at 6-12 months were frequently worse than comparison groups. For Achilles tendinopathy specifically, research has identified several concerning effects:
- Inhibition of collagen synthesis and tendon cell activity
- Reduced tendon mechanical properties (strength and stiffness)
- Increased risk of tendon rupture (estimated at 2-7%)
- Higher rates of symptom recurrence after initial relief
- Poorer long-term outcomes compared to exercise-based approaches
Rupture Risk
Multiple case studies and cohort analyses have documented Achilles tendon ruptures occurring within weeks to months following corticosteroid injection. This risk appears highest when injections are placed directly into the tendon substance rather than around it, and when patients return to high-load activities shortly after injection while pain is masked but tendon integrity is compromised.
Current Clinical Recommendations
Based on accumulated evidence, most sports medicine and orthopedic organizations now recommend against corticosteroid injections for Achilles tendinopathy in most cases:
“For Achilles tendinopathy, we generally advise against corticosteroid injections due to the increased risk of tendon rupture and poorer long-term outcomes compared to progressive loading programs.”
— American Academy of Orthopaedic Surgeons, Position Statement
When injections are considered, current guidelines suggest:
- Reserving them for cases that have failed appropriate conservative management
- Using ultrasound guidance to avoid intratendinous injection
- Implementing strict post-injection activity modification
- Combining with (not replacing) progressive loading programs
- Considering alternative injection options (e.g., high-volume injections, PRP)
The steroid injection example perfectly illustrates how focusing solely on short-term outcomes (pain relief) while ignoring long-term tissue effects led to treatment recommendations that ultimately harmed many patients – a cautionary tale about the importance of comprehensive research interpretation.
Eccentric Exercise Misapplication: Right Treatment, Wrong Context
The story of eccentric exercise for Achilles tendinopathy illustrates how even effective treatments can be misapplied when research is interpreted without proper context. This case demonstrates that understanding not just what works, but when and how it works, is crucial for optimal outcomes.
The Alfredson Protocol Revolution
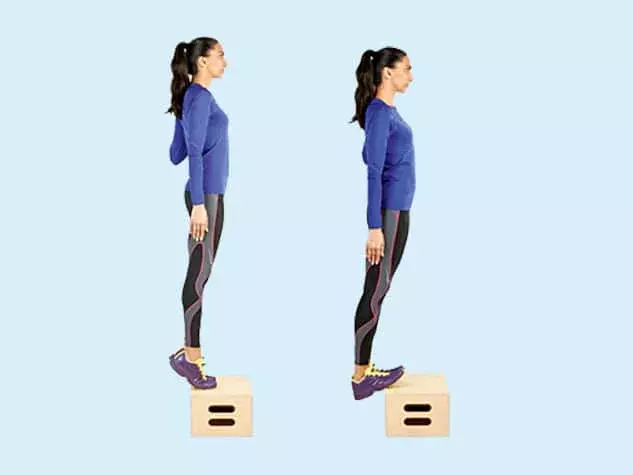
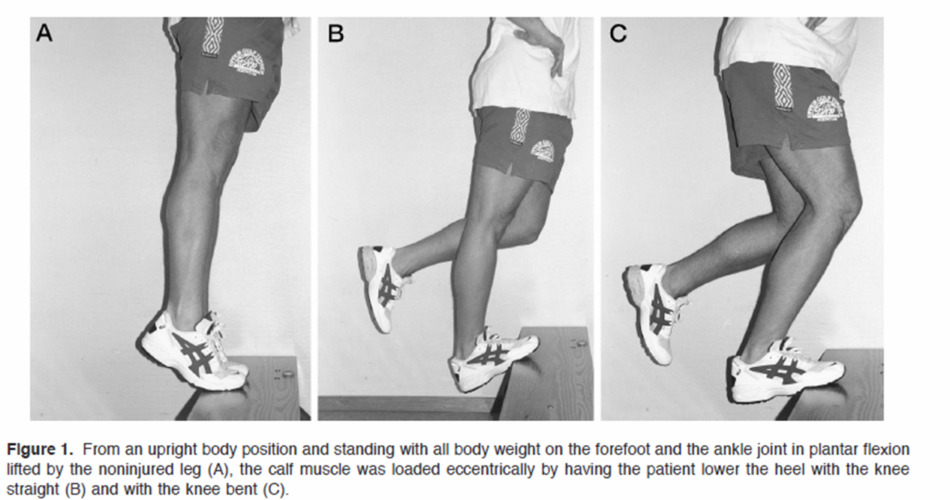
In 1998, Swedish researcher Håkan Alfredson published a landmark study introducing a heavy-load eccentric calf exercise program for mid-portion Achilles tendinopathy. The protocol involved performing heel drops off a step – lowering the heel below the step level while keeping the knee both straight and bent. The results were impressive: approximately 90% of patients with chronic mid-portion Achilles tendinopathy improved significantly after 12 weeks.
The Overgeneralization Problem
The success of Alfredson’s protocol led to widespread adoption of eccentric heel drops as the gold standard for all Achilles tendon problems. However, this generalization overlooked crucial details about the specific population studied:
- Participants had mid-portion tendinopathy (2-6cm above heel insertion)
- The study excluded insertional tendinopathy cases
- Subjects were able to tolerate the initial loading protocol
- The exercise was performed with specific parameters (3 sets of 15 reps, twice daily)
Despite these specifics, many clinicians began prescribing identical eccentric heel drops for all Achilles pain, regardless of location or presentation.
The Insertional Tendinopathy Problem
The misapplication became particularly problematic for patients with insertional Achilles tendinopathy (pain at the tendon-bone junction). Research by Jonsson and colleagues in 2008 revealed that the standard Alfredson protocol performed poorly for these patients:
| Protocol | Success Rate for Insertional Tendinopathy | Key Difference |
| Standard Alfredson (full range with heel below step) | Only 28% improvement | Creates compression at insertion point |
| Modified protocol (no heel drop below neutral) | 67% improvement | Avoids compression at insertion point |
The explanation for this difference lies in biomechanics. When the heel drops below the step level, the Achilles tendon gets compressed against the calcaneus (heel bone). In insertional tendinopathy, this compression exacerbates irritation at the already sensitive attachment point.
Beyond Eccentric-Only Approaches
Further research has revealed that the exclusive focus on eccentric contractions was also an oversimplification. Studies by Malliaras and others have shown that:
- Heavy slow resistance training (combining concentric and eccentric phases) produces similar outcomes
- Isometric exercises can provide immediate pain relief in reactive tendinopathy
- Different loading protocols may be appropriate for different stages of tendinopathy
- Individual response to specific exercise types varies significantly
Research Context Matters
The eccentric exercise case demonstrates why understanding research context is crucial. The Alfredson protocol works well for its intended population (mid-portion tendinopathy), but applying it universally without considering anatomical differences led to poor outcomes for many patients with insertional problems.
The lesson here parallels the “knees over toes” example – a valid finding (eccentric exercise helps mid-portion tendinopathy) was inappropriately generalized into a universal prescription, ignoring important contextual factors that determine its effectiveness.
Pain Avoidance Misconception: When “No Pain” Means “No Gain”
The relationship between pain and tissue damage is complex, especially in tendinopathy. A common misinterpretation of pain science has led many patients and practitioners to avoid any activity that produces discomfort – potentially hindering recovery in the process.
Origin of Pain Avoidance
The “avoid all pain” approach stems from a reasonable premise: pain signals potential harm, so activities that cause pain might be damaging tissues further. Early rehabilitation guidelines often emphasized pain-free movement, and the RICE protocol (Rest, Ice, Compression, Elevation) reinforced the idea that pain should be eliminated before resuming activity. This cautious approach made intuitive sense and aligned with patients’ natural desire to avoid discomfort.
The Pain-Damage Disconnect
Modern pain science has revealed that the relationship between pain and tissue damage is not straightforward, particularly in chronic conditions like tendinopathy. Research findings show:
- Pain levels often don’t correlate with the degree of tendon degeneration
- Some people with significant tendon changes on imaging have no pain
- Others with minimal visible changes experience severe pain
- Pain sensitivity can increase independently of tissue healing status
- The nervous system can become sensitized, lowering pain thresholds
This disconnect means that using pain as the sole guide for activity can be misleading. In tendinopathy, some pain during rehabilitation exercises may actually be necessary for optimal tendon adaptation and strengthening.
“In tendinopathy rehabilitation, the absence of all pain during exercise may indicate insufficient loading to stimulate positive tendon adaptation. Some discomfort during therapeutic exercise is often necessary and acceptable.”
— Jill Cook, PhD, Tendon Research Expert
The Pain Monitoring Approach
Current best practice has evolved from “avoid all pain” to “monitor and manage pain” during rehabilitation. Guidelines now suggest:
Acceptable Pain Levels
- Mild pain during exercise (3-4/10 on pain scale)
- Pain that doesn’t worsen during the activity
- Pain that returns to baseline within 24 hours
- No increase in morning stiffness the next day
Unacceptable Pain Signals
- Severe pain during activity (>5/10)
- Pain that worsens throughout the activity
- Pain that remains elevated 24 hours later
- Increased morning stiffness the following day
Consequences of Excessive Pain Avoidance
The misinterpretation that “all pain is bad” has led to several negative outcomes:
- Underloading tendons during rehabilitation
- Failure to progress exercises to therapeutic levels
- Development of fear-avoidance behaviors
- Prolonged recovery times
- Deconditioning of the tendon and surrounding tissues
By understanding that some discomfort during controlled rehabilitation is not only acceptable but often necessary, patients can achieve better outcomes. The key is distinguishing between productive pain (indicating appropriate challenge to the tissue) and counterproductive pain (signaling potential harm).
Overreliance on Passive Treatments: The Offloading Trap
Another common misinterpretation of Achilles tendinopathy research involves the role of passive treatments and offloading strategies. While devices like orthotics, heel lifts, and supportive footwear can play a valuable role in management, their benefits have often been overstated at the expense of active rehabilitation.
The Biomechanical Rationale
The emphasis on passive supports stems from valid biomechanical research. Studies have demonstrated that interventions like heel lifts can reduce Achilles tendon strain during walking and running. For example, a 12mm heel lift can decrease Achilles tendon force by approximately 25% during stance phase. This reduction in mechanical load seems beneficial, especially when the tendon is irritated.
The Misinterpretation
The problem arose when this mechanical offloading was viewed as a primary treatment rather than an adjunct to active rehabilitation. Many patients were prescribed expensive custom orthotics or told to permanently use heel lifts with the expectation that these devices alone would resolve their tendinopathy. The underlying misinterpretation was equating short-term load reduction with long-term healing.
This passive approach overlooked a fundamental principle of tissue adaptation: while temporary load reduction can help manage symptoms, the tendon ultimately needs progressive loading to regain its strength and function.
Benefits of Offloading
- Reduces pain during daily activities
- Makes exercise more tolerable
- Addresses contributing biomechanical factors
- Provides temporary symptom relief
Limitations of Offloading
- Doesn’t address underlying tendon weakness
- May lead to dependency on supports
- Can cause detraining in protected range
- Shifts stress to other structures
Research Reality Check
Systematic reviews examining orthotic interventions for Achilles tendinopathy have found limited evidence for their effectiveness as standalone treatments. While they may provide symptomatic relief, studies show that orthotics alone typically don’t lead to significant long-term improvements compared to exercise-based approaches.
The Balanced Approach
Current evidence supports using offloading strategies as part of a comprehensive management plan, not as the primary solution:
- Temporary heel lifts (6-12mm) to reduce pain during acute phases
- Supportive footwear to address contributing biomechanical factors
- Custom orthotics for cases with significant foot posture issues
- Gradual weaning from supports as tendon capacity improves
- Concurrent implementation of progressive loading exercises
Clinical Insight
Passive supports should be viewed as tools that create a window of opportunity for active rehabilitation, not as solutions in themselves. The goal should be to progressively reduce reliance on external support as the tendon’s intrinsic capacity improves.
This misinterpretation parallels the knee example – focusing exclusively on reducing mechanical stress (keeping knees behind toes or using heel lifts) without considering the importance of appropriate loading for tissue adaptation. The result in both cases was often weaker structures more vulnerable to future injury.
Evidence-Based Approaches: Current Best Practices for Achilles Tendinopathy
Having examined the common misinterpretations in Achilles tendinopathy research, let’s explore what current evidence actually supports. Modern approaches integrate the lessons learned from past misconceptions to create more effective, individualized treatment strategies.
The Load Management Framework
At the core of contemporary Achilles tendinopathy management is the concept of appropriate load management – finding the balance between too much and too little stress on the tendon. This approach recognizes that tendons need mechanical stimulation to adapt and strengthen, but excessive loading can overwhelm their capacity.
Stage-Appropriate Exercise Selection
Research now supports tailoring exercise selection to the specific stage and presentation of tendinopathy:
| Tendinopathy Stage | Recommended Exercise Approach | Clinical Reasoning |
| Reactive/Acute | Isometric holds, low-volume loading | Provides pain modulation with minimal irritation |
| Dysrepair/Mid-stage | Isotonic exercises, moderate volume | Begins rebuilding tendon capacity |
| Degenerative/Chronic | Heavy slow resistance, high-load training | Maximizes tendon remodeling and strength |
| Return to activity | Energy storage/release exercises | Prepares tendon for sport-specific demands |
Location-Specific Modifications
Learning from the eccentric exercise misapplication, current approaches differentiate between mid-portion and insertional Achilles tendinopathy:
Mid-Portion Tendinopathy
- Full range eccentric exercises can be beneficial
- Heel drops below step level are typically well-tolerated
- Higher volume protocols often effective (e.g., 3×15 twice daily)
- Can progress to plyometric activities as tolerated
Insertional Tendinopathy
- Avoid dorsiflexion beyond neutral position
- Perform heel raises/lowering on flat ground
- May benefit from temporary heel lift during daily activities
- Address any contributing compression factors
Pain-Guided Loading
Rather than avoiding all pain, current approaches use pain as a guide for appropriate loading:
- Mild pain during exercise (≤3/10) is acceptable
- Pain should not worsen throughout the exercise session
- Pain should return to baseline within 24 hours
- Morning stiffness should not increase the day after exercise
- Gradual progression based on symptom response, not rigid timelines
Comprehensive Management
Beyond exercise, evidence supports a multifaceted approach:
- Addressing contributing factors (training errors, footwear, biomechanics)
- Temporary load modification of aggravating activities
- Strategic use of supportive devices during rehabilitation
- Consideration of adjunct treatments for recalcitrant cases
- Education about tendon loading principles and pain science
Research Context Reminder
Even these current best practices must be applied with consideration of individual context. What works for a sedentary person with insertional tendinopathy will differ from what’s appropriate for an elite athlete with mid-portion issues. Treatment should always be individualized based on assessment findings, patient goals, and response to interventions.
Conclusion: Learning from Research Misinterpretations
The journey through Achilles tendinopathy research misinterpretations offers valuable lessons about how scientific findings can be distorted when taken out of context. Much like the “knees over toes” myth that restricted natural movement patterns for decades, these Achilles tendon misconceptions have led many patients down ineffective treatment paths.
Key Takeaways
As we’ve explored, several critical misinterpretations have shaped Achilles tendinopathy treatment:
- Complete rest is often counterproductive; tendons need appropriate loading to heal
- Chronic Achilles tendinopathy is primarily degenerative, not inflammatory
- Corticosteroid injections provide short-term relief but may worsen long-term outcomes
- Eccentric exercises work well for mid-portion tendinopathy but need modification for insertional cases
- Some pain during rehabilitation is acceptable and often necessary for adaptation
- Passive treatments like orthotics should complement, not replace, active loading programs
These misinterpretations share a common thread: they represent oversimplifications of complex research findings. In each case, a kernel of truth (rest reduces pain, inflammation plays some role, etc.) was exaggerated or applied without proper context, leading to suboptimal treatment approaches.
Finding Evidence-Based Care
- Seek healthcare providers who stay current with tendon research
- Be wary of one-size-fits-all approaches to Achilles tendinopathy
- Expect individualized assessment and treatment planning
- Look for practitioners who emphasize active rehabilitation over passive treatments
- Understand that recovery requires patience and consistent work – quick fixes rarely provide lasting results
The evolution of Achilles tendinopathy treatment reminds us that scientific understanding is always advancing. What seems like established fact today may be revised tomorrow as research methods improve and longer-term outcomes are studied. For patients and clinicians alike, maintaining a healthy skepticism about absolute claims and being open to emerging evidence is essential.
By learning from these research misinterpretations, we can approach Achilles tendinopathy with more nuanced, evidence-based strategies that balance immediate symptom management with long-term tendon health – ultimately leading to better outcomes and reduced recurrence of this challenging condition.
Consult a Specialist
If you’re dealing with Achilles tendon pain, consider consulting with a sports medicine physician, physical therapist, or podiatrist who specializes in tendinopathy. Look for providers who emphasize progressive loading approaches and individualized treatment plans based on current evidence.