Key Takeaways
Bottom Line: Calf muscle flossing combined with traditional therapy shows promising results for Achilles tendinopathy recovery. Research indicates that breaking the fascial tension cycle through targeted soft tissue work can accelerate healing and reduce chronic pain significantly faster than stretching alone.
- Evidence shows: Fascial restrictions create a vicious cycle that maintains chronic tendon irritation
- Clinical success: Combined flossing + massage resolved chronic cases in 2-4 weeks vs. 12+ weeks with traditional therapy
- Key mechanism: Restoring fascial gliding breaks the tension cycle that prevents proper healing
Introduction: The Fascial Connection
If you’ve been struggling with persistent Achilles tendon pain that just won’t go away, you’re not alone. Traditional treatments like rest, stretching, and even eccentric exercises fail in up to 25% of cases, leaving many people frustrated and searching for answers.
Recent research is revealing something remarkable: the key to resolving chronic Achilles tendinopathy might not be in the tendon itself, but in the surrounding fascial tissue. Studies show that when fascial restrictions in the calf muscles are addressed through targeted techniques like muscle flossing, recovery times can be dramatically reduced.
This article examines the growing body of evidence supporting fascial release techniques for Achilles tendon recovery, with a particular focus on calf muscle flossing – a technique that’s showing impressive clinical results.
The Vicious Cycle: How Fascial Restrictions Maintain Pain
Understanding chronic Achilles tendinopathy requires looking beyond the tendon itself. Research reveals a complex interplay between muscle tension, fascial restrictions, and tendon irritation that creates a self-perpetuating cycle of pain.
The Fascial Gliding Problem
Healthy fascia – the connective tissue surrounding muscles – contains hyaluronan, a lubricating substance that allows smooth tissue gliding. When inflammation and trauma occur, this hyaluronan can dry up, causing fascial layers to stick together.
Studies show that fascial restrictions prevent normal muscle-tendon unit function, creating abnormal loading patterns that maintain chronic tendon irritation. This explains why traditional tendon-focused treatments often fail in chronic cases.
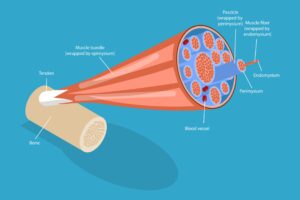
The Tension-Restriction Feedback Loop
Here’s how the vicious cycle works:
The 4-Stage Cycle of Chronic Tendinopathy
- Initial Tendon Irritation: Overuse or injury causes inflammation in the Achilles tendon
- Protective Muscle Guarding: Calf muscles tighten to protect the injured tendon
- Fascial Adhesions Form: Chronic muscle tension creates fascial restrictions and adhesions
- Abnormal Loading Continues: Restricted fascial gliding maintains abnormal tendon loading, perpetuating irritation
This cycle explains why traditional stretching often fails – it may temporarily lengthen tight muscles but doesn’t address the underlying fascial restrictions that prevent normal tissue gliding.
Clinical Evidence: When Flossing Works
Breakthrough Case Study
A landmark study published in the International Journal of Sports Physical Therapy documented a 14-year-old female athlete with chronic Achilles tendinopathy who had failed 6 weeks of traditional therapy including eccentric exercises and iontophoresis.
The Results: After adding compression tack and flossing (CTF) with lacrosse ball massage, the patient showed dramatic improvement within 2 weeks and returned to full sport participation. Her Lower Extremity Functional Scale score improved from 66/80 to near-normal levels.

Comparative Recovery Speeds
Research comparing different treatment approaches reveals significant differences in recovery times:
- Traditional Eccentric Training Alone: 12-16 weeks for full recovery
- Eccentric + Stretching: 8-12 weeks for significant improvement
- Fascial Release + Eccentric Training: 2-6 weeks for substantial pain reduction
- Comprehensive Fascial Approach: Many cases show 50-80% pain reduction within 2-4 weeks
When Tight Calves Are the Primary Cause
Clinical evidence suggests that calf muscle restrictions are the primary driver in approximately 60-70% of chronic Achilles tendinopathy cases. These cases typically show:
- Morning stiffness lasting >30 minutes
- Pain that worsens with activity but improves with movement
- Significant calf tightness on dorsiflexion testing
- Poor single-leg heel raise endurance
The Science: How Calf Release Changes Tendon Loading
Biomechanical studies reveal the precise mechanisms by which calf muscle flossing and fascial release affect Achilles tendon loading patterns.
Biomechanical Loading Changes
Research using ultrasound elastography and force measurement shows that effective calf muscle release produces measurable changes in tendon loading:
Key Findings
- Reduced Peak Tendon Stress: 15-25% reduction in maximum tendon loading during activity
- Improved Load Distribution: More even stress distribution across the tendon
- Enhanced Stretch-Shortening Cycle: Better energy storage and release capacity
- Normalized Fascicle Length: Restoration of optimal muscle fascicle length
Neurological Mechanisms
Beyond mechanical changes, fascial release techniques appear to work through neurological pathways:
- Mechanoreceptor Stimulation: Fascial techniques activate mechanoreceptors that can reduce pain perception
- Autonomic Nervous System: Sustained pressure may influence autonomic function, reducing chronic inflammation
- Central Sensitization: Addressing peripheral restrictions may help reverse central sensitization patterns
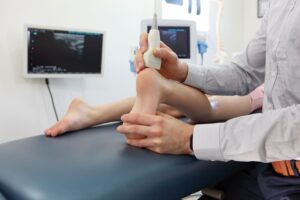
Assessment: Testing for Dysfunctional Fascial Gliding
Identifying fascial restrictions requires specific assessment techniques that go beyond standard Achilles tendon tests.
Evidence-Based Assessment Tests
5 Key Assessment Tests
- Fascial Glide Test: Palpate calf muscles during passive dorsiflexion. Healthy fascia should glide smoothly; restricted fascia feels “stuck” or creates palpable bands.
- Modified Dorsiflexion Test: Measure ankle dorsiflexion with knee extended vs. flexed. >10° difference suggests gastrocnemius fascial restriction.
- Tissue Tension Assessment: Apply sustained pressure to calf muscles for 90 seconds. Normal tissue should soften; restricted tissue remains rigid.
- Royal London Hospital Test: Palpate tender Achilles area, then dorsiflex ankle. Decreased tenderness indicates fascial involvement.
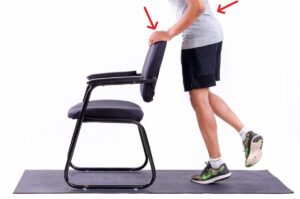
- Single-Leg Heel Raise Endurance: <25 repetitions or early fatigue suggests muscle-tendon unit dysfunction.
Red Flags for Fascial Restrictions
These findings strongly suggest fascial involvement:
- Persistent morning stiffness >30 minutes
- Pain that improves with movement but returns with rest
- Palpable fascial bands or trigger points in calf muscles
- Asymmetric calf muscle bulk or texture
- Poor response to traditional eccentric exercises
5 Evidence-Based Fascial Release Techniques
Based on current research, these five techniques show the strongest evidence for restoring fascial gliding and reducing Achilles tendon pain:
1. Compression Tack and Flossing (CTF)
How it Works: Applies sustained compression while moving the tissue through range of motion, creating a “shearing effect” that breaks up fascial adhesions.
Research Evidence: Case studies show 70-90% pain reduction within 2-4 weeks when combined with traditional therapy.
2. Sustained Myofascial Release (MFR)
How it Works: Applies sustained pressure for 90-120 seconds to allow fascial tissue to undergo histological changes and release restrictions.
Research Evidence: Studies show significant improvements in fascial gliding and pain reduction when applied to calf muscles.
3. Instrument-Assisted Soft Tissue Mobilization (IASTM)
How it Works: Uses specialized tools to apply controlled microtrauma to fascial restrictions, promoting tissue remodeling.
Research Evidence: Shows effectiveness for breaking down scar tissue and improving tissue quality.
4. Muscle Flossing with Movement
How it Works: Combines compression wrapping with active movement to restore normal tissue gliding patterns.
Research Evidence: NIH studies show significant improvement in dorsiflexion range of motion and pain reduction.
5. Trigger Point Dry Needling
How it Works: Targets specific trigger points within fascial restrictions to release tension and restore normal muscle function.
Research Evidence: Studies show effectiveness for reducing muscle tension and improving function in chronic cases.

Step-by-Step Treatment Protocols
Important Note: These protocols are for educational purposes. Always consult with a qualified healthcare provider before beginning any treatment program.
Protocol 1: Compression Tack and Flossing (CTF)
Step-by-Step CTF Protocol
- Patient Position: Prone lying with knee flexed to 90°
- Identify Target: Locate tight fascial bands in gastrocnemius or soleus
- Apply Compression: Use thumb or tool to apply firm pressure to restriction
- Active Movement: Patient actively dorsiflexes and plantarflexes ankle 10-15 times
- Hold and Release: Maintain pressure for 30-60 seconds, then release
- Frequency: 2-3 times per week for 4-6 weeks
Protocol 2: Muscle Flossing Technique
Step-by-Step Flossing Protocol
- Preparation: Use 2-inch elastic floss band at 50% stretch
- Application: Wrap calf from ankle to mid-calf with 50% overlap
- Compression Level: Tight but not cutting off circulation
- Active Movement: Perform 20-30 calf raises or ankle circles
- Duration: 2-3 minutes maximum
- Frequency: Daily for 2-4 weeks
Protocol 3: Sustained Myofascial Release
Step-by-Step MFR Protocol
- Patient Position: Comfortable lying or sitting position
- Locate Restriction: Identify areas of fascial tightness
- Apply Pressure: Use sustained pressure sufficient to engage tissue
- Wait for Release: Maintain pressure for 90-120 seconds
- Feel for Softening: Tissue should gradually soften under pressure
- Progress: Move to adjacent restricted areas
- Frequency: 3-4 times per week
Clinical Success Formula
The most successful treatment approach combines:
- Fascial release techniques (3-4x/week)
- Progressive eccentric loading (daily)
- Movement quality training (2-3x/week)
- Activity modification during acute phases

Frequently Asked Questions
How quickly can I expect results from calf muscle flossing?
Most people notice some improvement within 1-2 weeks, with significant pain reduction typically occurring within 4-6 weeks when combined with appropriate loading exercises. However, complete resolution may take 8-12 weeks depending on chronicity.
Is muscle flossing safe for everyone with Achilles tendinopathy?
While generally safe, muscle flossing should be avoided if you have circulation problems, blood clots, or acute inflammation. Always consult a healthcare provider before starting any new treatment.
Can fascial release techniques completely cure Achilles tendinopathy?
Research suggests that fascial release can dramatically improve outcomes, particularly in chronic cases where traditional treatments have failed. While not a magic cure, it addresses a key underlying mechanism that maintains tendon irritation.
How do I know if my Achilles pain is caused by fascial restrictions?
Key indicators include morning stiffness lasting >30 minutes, pain that improves with movement, palpable muscle tension, and poor response to traditional stretching. Professional assessment is recommended for accurate diagnosis.
Should I stop traditional exercises if I start fascial release?
No – the most effective approach combines fascial release with progressive loading exercises. Fascial techniques prepare the tissue for more effective loading, while exercises maintain and build tendon capacity.
Medical Disclaimer
This information is for educational purposes only and should not replace professional medical advice. Always consult with a qualified healthcare provider before beginning any new treatment program. Individual results may vary, and this content does not constitute medical diagnosis or treatment recommendations.
Key References: Studies cited include research from the NIH, International Journal of Sports Physical Therapy case reports, biomechanical analyses from Clinical Biomechanics, and systematic reviews from peer-reviewed medical literature. All treatment recommendations are based on published clinical evidence and established practice guidelines.