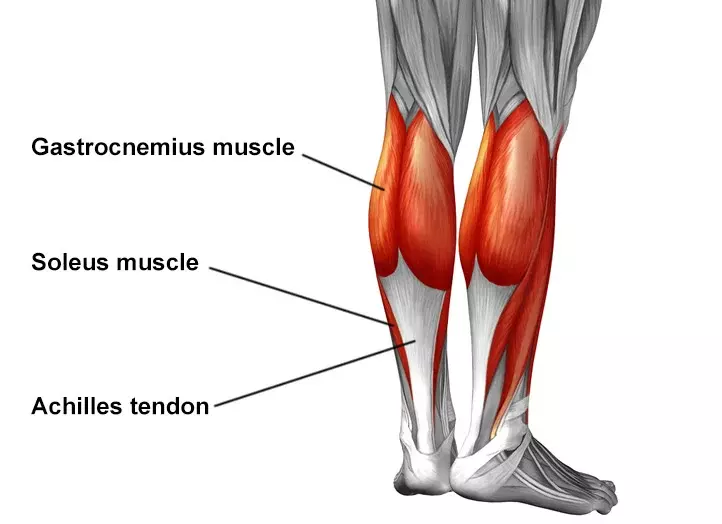
The Achilles tendon, connecting your calf muscles to your heel bone, plays a crucial role in everyday movement. When this tendon hurts, it can significantly impact your mobility and quality of life. But how do you know when Achilles tendon pain requires medical attention versus home care? This comprehensive guide will help you understand the causes of Achilles tendon pain, recognize warning signs that indicate serious issues, and make informed decisions about when to seek professional medical care.
| Contents | Jump to Section |
| What Causes Achilles Tendon Pain? | Read More |
| When Is Achilles Pain Serious? Red Flags to Watch | Read More |
| When to See a Doctor: Clinical Guidelines | Read More |
| Diagnosing Achilles Tendon Conditions | Read More |
| Home Care vs Medical Treatment | Read More |
| Risks of Delaying Treatment | Read More |
| Post-Diagnosis Next Steps | Read More |
| FAQs: Getting Help for Achilles Pain | Read More |
What Causes Achilles Tendon Pain?
Understanding the underlying causes of Achilles tendon pain is essential for determining when medical attention is necessary. The Achilles tendon bears significant stress during everyday activities and can develop various conditions that cause discomfort.
Overuse Injuries: Tendonitis and Tendinopathy
The most common causes of Achilles tendon pain are overuse injuries. These typically develop gradually as the tendon experiences repeated stress without adequate recovery time.
Achilles Tendonitis
Achilles tendonitis occurs when the tendon becomes inflamed due to excessive stress. This condition is characterized by:
- Pain and stiffness along the tendon, especially in the morning
- Swelling that worsens throughout the day
- Increased discomfort after activity
- Tenderness when touched
Achilles Tendinopathy
Tendinopathy is a degenerative condition where the tendon tissue breaks down over time. Unlike tendonitis, it’s not primarily inflammatory. Signs include:
- Persistent pain that doesn’t improve with rest
- Thickening of the tendon
- Formation of nodules or lumps in the tendon
- Reduced strength and flexibility
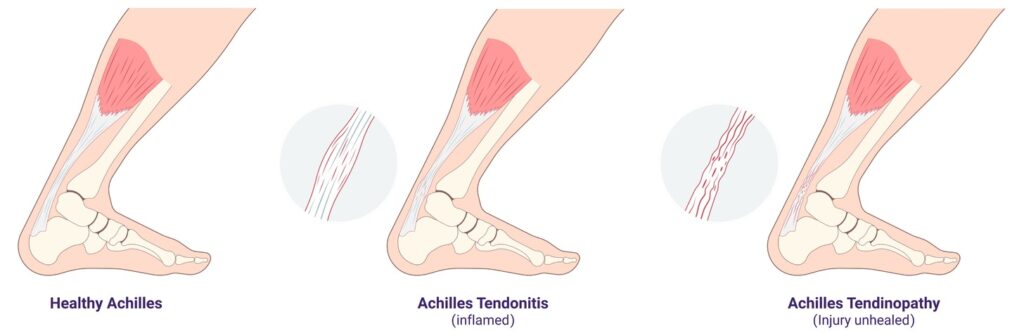
Acute vs. Chronic Inflammation
Achilles tendon pain can be categorized based on its duration and development:
Acute Inflammation
Acute inflammation develops suddenly, often after a specific incident or activity. It typically causes:
- Sharp, intense pain
- Noticeable swelling and redness
- Warmth around the affected area
- Symptoms that develop within hours or days
Chronic Inflammation
Chronic inflammation develops gradually over weeks or months and is characterized by:
- Persistent, dull aching
- Morning stiffness that improves with movement
- Thickening of the tendon over time
- Pain that fluctuates but never fully resolves
Ruptures and Partial Tears
More severe Achilles tendon injuries include partial tears and complete ruptures. These typically occur during high-impact activities or when the tendon is already weakened.
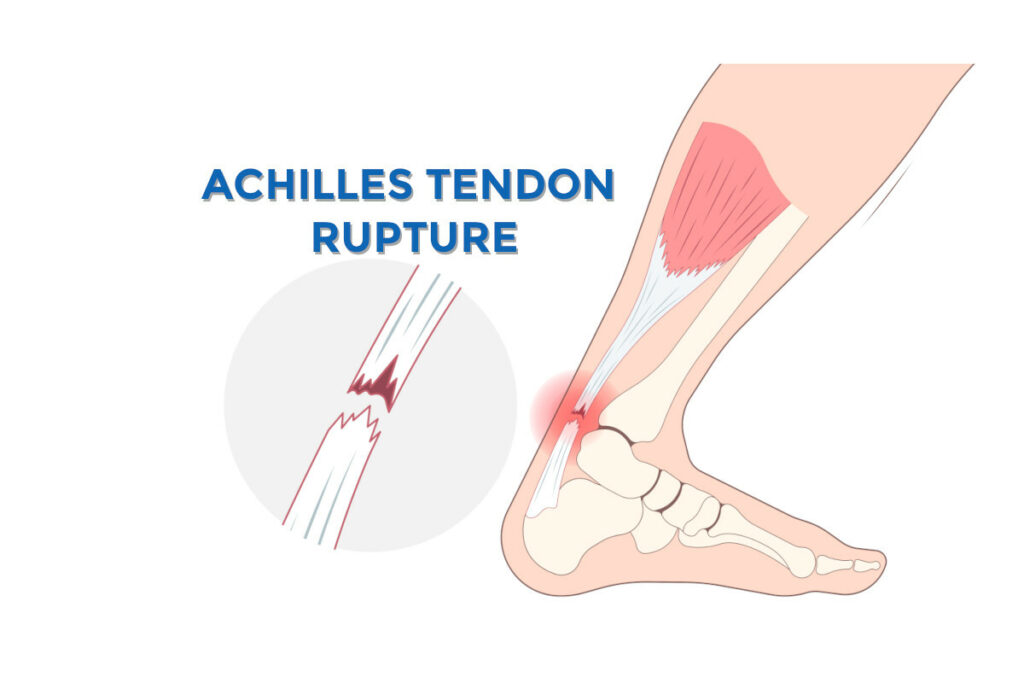
An Achilles tendon rupture often produces:
- A sudden “pop” or snapping sensation in the back of the leg
- Immediate, severe pain
- Inability to stand on tiptoes or push off when walking
- Visible gap in the tendon
- Significant swelling and bruising
Biomechanical and Age-Related Factors
Several factors can increase your risk of developing Achilles tendon pain:
Biomechanical Factors
- Flat feet or overpronation
- High arches
- Tight calf muscles
- Leg length discrepancy
- Poor footwear with inadequate support
Age-Related Factors
- Natural tendon degeneration after age 30
- Reduced blood flow to tendons
- Decreased elasticity in tendon tissue
- Longer recovery time after activity
When Is Achilles Pain Serious? Red Flags to Watch
While many cases of Achilles tendon pain can be managed at home, certain symptoms indicate a more serious condition that requires prompt medical attention. Recognizing these red flags can help prevent complications and ensure proper treatment.
Urgent Warning Signs
Seek immediate medical attention if you experience any of the following:
- A sudden “pop” or snapping sensation in your Achilles area
- Inability to bear weight on the affected foot
- Severe pain that makes walking impossible
- Visible deformity or gap in the tendon
- Significant swelling or bruising
Sudden Pop or Snap
A sudden popping or snapping sensation in the back of your leg is often the first sign of an Achilles tendon rupture. This sensation typically occurs during activities that place sudden stress on the tendon, such as:
- Pushing off suddenly when starting to run
- Jumping or landing from a jump
- Quickly changing direction during sports
- Falling or stumbling unexpectedly
Sharp Pain or Inability to Push Off
Severe, sharp pain in the Achilles tendon area that prevents normal movement requires medical evaluation. Pay particular attention if you:
- Cannot stand on your tiptoes on the affected side
- Experience pain that doesn’t improve with rest
- Feel a sharp, stabbing sensation with each step
- Cannot push off with your foot when walking
Swelling or Bruising
While mild swelling can occur with minor Achilles tendon issues, significant swelling or bruising indicates a more serious injury. Concerning signs include:
- Rapid onset of swelling within hours of injury
- Bruising that extends down toward the heel or up the calf
- Swelling that doesn’t improve after 2-3 days of RICE (Rest, Ice, Compression, Elevation)
- Warmth and redness accompanying the swelling
Long-Term Pain with No Improvement
Persistent Achilles tendon pain that doesn’t respond to home care measures should not be ignored. Seek medical attention if you experience:
- Pain lasting more than 2-3 weeks despite rest and home treatment
- Pain that initially improves but then returns or worsens
- Night pain that disturbs sleep
- Pain accompanied by stiffness that doesn’t improve throughout the day
When to See a Doctor: Clinical Guidelines & Recommendations
Knowing exactly when to seek medical care for Achilles tendon pain can be challenging. These evidence-based guidelines will help you make informed decisions about when professional evaluation is necessary.
How Long to Wait with Mild Symptoms
For mild Achilles tendon pain without the red flags mentioned above, you can typically try home care measures first:
| Symptom Severity | Recommended Waiting Period | When to Seek Care |
| Mild discomfort | 1-2 weeks of home care | If no improvement or worsening symptoms |
| Moderate pain affecting daily activities | 3-5 days of home care | If pain persists or limits normal walking |
| Pain with visible swelling | 1-2 days of RICE protocol | If swelling doesn’t subside or pain increases |
| Any red flag symptoms | Seek immediate care | Same day or emergency care |
When to Go to Urgent Care vs. Orthopedist
The type of medical care you seek depends on the nature and severity of your symptoms:
Seek Urgent Care When:
- You experience sudden, severe pain
- You hear or feel a “pop” in your Achilles tendon
- You cannot walk or bear weight on the affected foot
- You have significant swelling or bruising
- The injury occurred within the past 24-48 hours
See an Orthopedist or Podiatrist When:
- You have persistent pain lasting more than 2 weeks
- Home treatments haven’t improved symptoms
- Pain recurs after initial improvement
- You have chronic tendon issues
- You need specialized treatment or rehabilitation
Importance of Early Diagnosis for Long-Term Outcome
Research consistently shows that early diagnosis and appropriate treatment of Achilles tendon injuries lead to better outcomes. According to a 2021 study published in the Journal of Orthopaedic Surgery and Research, patients who received treatment within two weeks of injury had:
- Faster return to normal activities
- Lower rates of chronic tendon problems
- Reduced need for surgical intervention
- Better long-term tendon function
- Lower risk of re-injury
Symptoms Requiring MRI or Ultrasound
Certain symptoms indicate the need for advanced imaging to properly diagnose your condition:
- Suspected tendon rupture or significant tear
- Persistent pain despite appropriate treatment
- Significant swelling or thickening of the tendon
- History of multiple Achilles tendon injuries
- Unusual symptoms that don’t fit typical patterns
Professional Tip
When making an appointment, be specific about your symptoms and their duration. Mention any “popping” sensation, inability to bear weight, or significant swelling, as these symptoms may warrant more urgent evaluation.
Diagnosing Achilles Tendon Conditions: What to Expect
When you visit a healthcare provider for Achilles tendon pain, they’ll use several methods to diagnose your condition accurately. Understanding this process can help you prepare for your appointment and ensure you receive the most appropriate care.
Physical Exam Tests
Your healthcare provider will likely perform several physical examination tests to assess your Achilles tendon:
Thompson Test (Calf Squeeze Test)
This test helps diagnose Achilles tendon ruptures:
- You’ll lie face down with your feet hanging off the examination table
- The doctor will squeeze your calf muscle
- In a healthy tendon, this causes the foot to point downward
- If the foot doesn’t move, it may indicate a ruptured Achilles tendon
Range of Motion Assessment
Your provider will evaluate:
- How far you can point your foot up and down
- Whether movement causes pain
- If there are limitations in specific directions
- Differences between your affected and unaffected sides
Palpation
Your provider will carefully feel your Achilles tendon to check for:
- Tenderness or pain when touched
- Thickening or nodules in the tendon
- Gaps that might indicate a tear or rupture
- Warmth or swelling around the tendon
Imaging (MRI, Ultrasound, X-ray)
Depending on your symptoms and physical examination findings, your provider may recommend imaging tests:
| Imaging Type | What It Shows | When It’s Used |
| Ultrasound | Tendon structure, tears, inflammation | First-line imaging for most Achilles tendon issues |
| MRI | Detailed view of tendon, surrounding tissues | Complex cases, surgical planning, unclear diagnosis |
| X-ray | Bone spurs, calcification, bone injuries | To rule out bone-related causes of heel pain |
Referrals and Second Opinions
Depending on your initial evaluation, you may be referred to specialists:
- Orthopedic surgeon: For surgical evaluation of severe tendon injuries
- Sports medicine specialist: For activity-related tendon issues
- Physical therapist: For rehabilitation and strengthening programs
- Podiatrist: For foot-related biomechanical issues contributing to tendon pain
When to Consider a Second Opinion
Consider seeking a second opinion if:
- Your symptoms don’t match your diagnosis
- Your treatment isn’t producing expected results
- Surgery is recommended for a non-emergency condition
- You want to explore all treatment options
Home Care vs Medical Treatment: What’s Appropriate?
Understanding when self-care is sufficient and when professional medical treatment is necessary can help you manage Achilles tendon pain effectively while avoiding complications.
Appropriate Home Care Measures
For mild to moderate Achilles tendon pain without red flag symptoms, these home care strategies may be appropriate:
RICE Method
- Rest: Reduce activities that cause pain, especially high-impact exercises
- Ice: Apply ice for 15-20 minutes several times daily
- Compression: Use an elastic bandage to reduce swelling
- Elevation: Keep your foot elevated above heart level when possible
Gentle Movement and Stretching
Once acute pain subsides:
- Gentle calf stretches to maintain flexibility
- Ankle range-of-motion exercises
- Low-impact activities like swimming or cycling
- Gradual return to normal activities as pain allows
Supportive Footwear and Modifications
- Shoes with good arch support and cushioning
- Heel lifts to reduce tendon strain
- Avoiding barefoot walking
- Temporary use of a walking boot for more severe pain
Limitations of Self-Care
While home care is appropriate for minor issues, it has important limitations:
When Home Care Is Not Enough
Self-care is insufficient and medical care should be sought when:
- Pain is severe or worsening despite home treatment
- You experience any red flag symptoms (pop, inability to bear weight, etc.)
- Symptoms persist for more than 2 weeks with proper home care
- You’re unable to perform normal daily activities
- You have medical conditions that affect healing (diabetes, peripheral vascular disease)
When Conservative Care Fails
If appropriate home care and initial medical treatments don’t resolve your symptoms, your healthcare provider may recommend:
Advanced Non-Surgical Treatments
- Physical therapy with specialized protocols
- Custom orthotic devices
- Extracorporeal shockwave therapy
- Platelet-rich plasma injections
- Specialized bracing or taping techniques
Surgical Interventions
- Tendon debridement (removal of damaged tissue)
- Tendon repair for partial tears
- Tendon reconstruction for complete ruptures
- Removal of bone spurs if present
- Lengthening of tight calf muscles
“The decision between conservative and surgical management should be individualized based on the patient’s age, activity level, and the nature and severity of the tendon injury.”
— American Academy of Orthopaedic Surgeons, 2022
What Happens If You Wait Too Long? Risks of Delay
Delaying appropriate treatment for Achilles tendon pain can lead to serious complications and poorer outcomes. Understanding these risks can help motivate timely care when needed.
Chronic Tendinopathy
Without proper treatment, acute Achilles tendon issues can evolve into chronic conditions that are more difficult to resolve:
- Tendon fibers become permanently disorganized and weakened
- Blood flow to the tendon decreases, slowing healing
- Scar tissue forms, reducing flexibility and function
- Pain becomes persistent and less responsive to treatment
- Recovery time extends from weeks to months or even years
Higher Re-Injury Rates
Untreated or improperly treated Achilles tendon injuries significantly increase the risk of future problems:
- Weakened tendon structure is more vulnerable to new injuries
- Compensatory movement patterns stress other structures
- Biomechanical issues that caused the initial problem worsen
- Return to activities becomes increasingly difficult
- Each re-injury typically requires longer recovery time
Loss of Function
Prolonged Achilles tendon problems can lead to significant functional limitations:
Short-Term Functional Loss
- Difficulty walking, especially on uneven surfaces
- Inability to participate in sports or exercise
- Challenges with stairs and inclines
- Pain with daily activities
Long-Term Functional Loss
- Permanent gait alterations
- Chronic pain with activity
- Reduced ankle range of motion
- Inability to return to previous activity levels
Surgery Becoming Necessary
What might have been treated conservatively can progress to requiring surgical intervention:
- Complete ruptures from weakened tendons often require surgical repair
- Extensive tendon degeneration may need debridement or reconstruction
- Surgical outcomes are typically better when performed earlier
- Recovery from surgery is longer and more involved than from conservative care
- Surgical complications become more likely with advanced tendon damage
Research Findings on Delayed Treatment
According to a 2022 study in the Journal of Orthopaedic & Sports Physical Therapy, patients who delayed treatment for Achilles tendon issues by more than 4 weeks had:
- 42% longer recovery times
- 3.5 times higher risk of developing chronic symptoms
- 2.8 times greater likelihood of requiring surgical intervention
- Significantly lower satisfaction with treatment outcomes
Post-Diagnosis: What Are Your Next Steps?
After receiving a diagnosis for your Achilles tendon condition, understanding your treatment options and recovery path is essential. Here’s what to expect based on different diagnoses.
Conservative Management
For most non-rupture Achilles tendon conditions, conservative treatment is the first approach:
Initial Phase (1-2 weeks)
- RICE protocol (Rest, Ice, Compression, Elevation)
- Activity modification to reduce tendon stress
- Over-the-counter anti-inflammatory medications if recommended
- Supportive footwear or temporary walking boot
- Gentle range-of-motion exercises as pain allows
Rehabilitation Phase (2-8 weeks)
- Progressive strengthening exercises
- Eccentric calf exercises (shown to be particularly effective)
- Gradual return to weight-bearing activities
- Continued use of supportive devices as needed
- Addressing biomechanical issues with proper footwear or orthotics
Return to Activity Phase (8-12+ weeks)
- Sport-specific or activity-specific training
- Continued strengthening and flexibility exercises
- Gradual increase in activity intensity and duration
- Maintenance program to prevent recurrence
- Regular monitoring for any symptom return
Rehab and PT Referrals
Physical therapy plays a crucial role in Achilles tendon recovery:
What to Expect from PT
- Comprehensive evaluation of your condition
- Customized exercise program
- Manual therapy techniques
- Education on proper movement patterns
- Guidance on activity modification
How to Maximize PT Benefits
- Attend all scheduled sessions
- Consistently perform home exercises
- Communicate changes in symptoms
- Follow activity restrictions
- Ask questions about your recovery
Surgical Consultation Timelines
If surgery is recommended or being considered, understanding the timeline helps set expectations:
| Condition | Surgical Urgency | Typical Timeline |
| Complete rupture | High | Within 1-2 weeks of injury for optimal outcomes |
| Partial tear | Moderate | After 4-6 weeks of failed conservative treatment |
| Chronic tendinopathy | Low | After 3-6 months of failed conservative treatment |
| Insertional tendinopathy with bone spur | Low to moderate | After 3+ months of failed conservative treatment |
Questions to Ask Your Doctor
When discussing your treatment plan, consider asking:
- What is my specific diagnosis and its severity?
- What are all my treatment options?
- What is the expected recovery timeline?
- What activity restrictions should I follow?
- What signs indicate I’m improving or worsening?
- When can I return to my normal activities?
- How can I prevent this from happening again?
FAQs: Getting Help for Achilles Tendon Pain
How do I know if my Achilles tendon is torn or just strained?
A torn (ruptured) Achilles tendon typically produces:
- A sudden “pop” or snapping sensation
- Immediate, severe pain
- Inability to stand on tiptoes or push off when walking
- Visible gap or indentation in the tendon
- Significant swelling and bruising
A strain usually causes more gradual pain, mild to moderate swelling, and some limitation in movement but not complete inability to push off. When in doubt, seek medical evaluation, as proper diagnosis is crucial for appropriate treatment.
Can I still walk with Achilles tendonitis?
Yes, most people with Achilles tendonitis can still walk, though you may experience pain and discomfort, especially when first standing after rest. However, continuing to walk normally with significant pain can worsen the condition. Consider:
- Temporarily reducing walking distance and intensity
- Using supportive footwear with a slight heel lift
- Avoiding hills, uneven surfaces, and stairs when possible
- Using a walking boot if recommended by your healthcare provider
If walking causes moderate to severe pain, seek medical advice before continuing regular activities.
How long does it take for Achilles tendon pain to go away?
Recovery time varies based on the condition’s severity and the treatment approach:
- Mild tendonitis: 2-3 weeks with proper rest and care
- Moderate tendinopathy: 6-8 weeks with appropriate treatment
- Severe tendinopathy: 3-6 months of consistent rehabilitation
- Partial tear: 3-6 months with conservative treatment
- Complete rupture (surgical repair): 4-6 months for full recovery
- Complete rupture (non-surgical): 6-12 months for full recovery
These timeframes assume appropriate treatment and compliance with rehabilitation protocols. Continuing activities that stress the tendon can significantly extend recovery time.
What type of doctor should I see for Achilles tendon pain?
Several types of healthcare providers can evaluate and treat Achilles tendon pain:
- Primary care physician: Good starting point for initial evaluation and referrals
- Orthopedic surgeon: Specializes in musculoskeletal conditions and surgical interventions
- Sports medicine physician: Focuses on activity-related injuries and non-surgical management
- Podiatrist: Specializes in foot and ankle conditions, including Achilles tendon issues
- Physical medicine and rehabilitation (PM&R) physician: Focuses on non-surgical treatment and rehabilitation
For acute injuries with severe pain or suspected rupture, start with an urgent care center or emergency department for immediate evaluation.
Can I treat Achilles tendon pain at home?
Mild Achilles tendon pain can often be initially managed at home with:
- RICE protocol (Rest, Ice, Compression, Elevation)
- Over-the-counter anti-inflammatory medications (if not contraindicated)
- Activity modification to reduce stress on the tendon
- Supportive footwear with cushioning and slight heel lift
- Gentle stretching once acute pain subsides
However, seek medical care if:
- Pain is severe or worsening
- You experience any red flag symptoms
- Symptoms don’t improve after 1-2 weeks of home care
- You have medical conditions that affect healing
Will I need surgery for my Achilles tendon injury?
The need for surgery depends on several factors:
- Complete ruptures: Often benefit from surgical repair, especially in younger, active individuals
- Partial tears: May heal with conservative treatment but sometimes require surgery if they don’t improve
- Chronic tendinopathy: Surgery is typically considered only after 3-6 months of failed conservative treatment
- Insertional tendinopathy with bone spurs: May require surgery to remove bone spurs if conservative measures fail
Your age, activity level, overall health, and specific condition all factor into the decision. Always discuss the potential benefits and risks of surgical versus non-surgical approaches with your healthcare provider.
Conclusion: Don’t Ignore the Warning Signs
Achilles tendon pain can range from a minor nuisance to a serious injury requiring immediate medical attention. Understanding when to seek professional care is crucial for optimal recovery and preventing long-term complications.
Key Takeaways
- Seek immediate medical attention for sudden pops, inability to bear weight, or severe pain
- Don’t ignore persistent Achilles pain that doesn’t improve with basic home care
- Early diagnosis and appropriate treatment lead to better outcomes and faster recovery
- Follow your healthcare provider’s recommendations for activity modification and rehabilitation
- Take preventive measures to protect your Achilles tendon during physical activities
Remember that while many cases of Achilles tendon pain can be successfully treated with conservative measures, delaying appropriate care when it’s needed can lead to chronic problems, longer recovery times, and potentially more invasive treatments. Listen to your body, respect pain as a warning sign, and seek professional guidance when red flags appear.
By understanding the causes of Achilles tendon pain, recognizing warning signs, and knowing when to seek medical care, you can take control of your tendon health and make informed decisions about your treatment and recovery.